Vaccination against COVID-19 started in many countries and it has become the ray of hope to control this ongoing pandemic. But those who suffered and recovered from the disease, many of them consulted the doctors for post covid complications such as mucormycosis, candida, and other odd infections also.
Today we have an interesting case study that was shared by Dr. Pratik Savaj who is an infectious disease specialist serving in the Surat city of Gujarat, India. Let’s have a look at our interesting case study of oral ulcers.
Table of Contents
An interesting case of Post covid complications herpes ulcer and oesophagitis
A 62 your male patient diagnosed with COVID-19 with no comorbid conditions. On the day 5th from the onset of symptoms, he become hypoxic.
Therefore dexamethasone with remdesivir started. He was slowly improving and CRP was seriously going down. He required dexamethasone for 7 days.
On day 7th his CRP level started rising again. He has lots of oral ulcers and dysphagia.
Candidiasis is the most common infection that a patient encounters which represents as oral ulcers. Intravenous fluconazole started owing to this consideration. But there was no improvement in the complaint of the patient.
Repeat HRCT (CT scan of Thorax) done and it was again static.
The ulcers were very painful and dysphagia was very severe. All kinds of Vitamin preparation were started but there was no significant result and improvement.
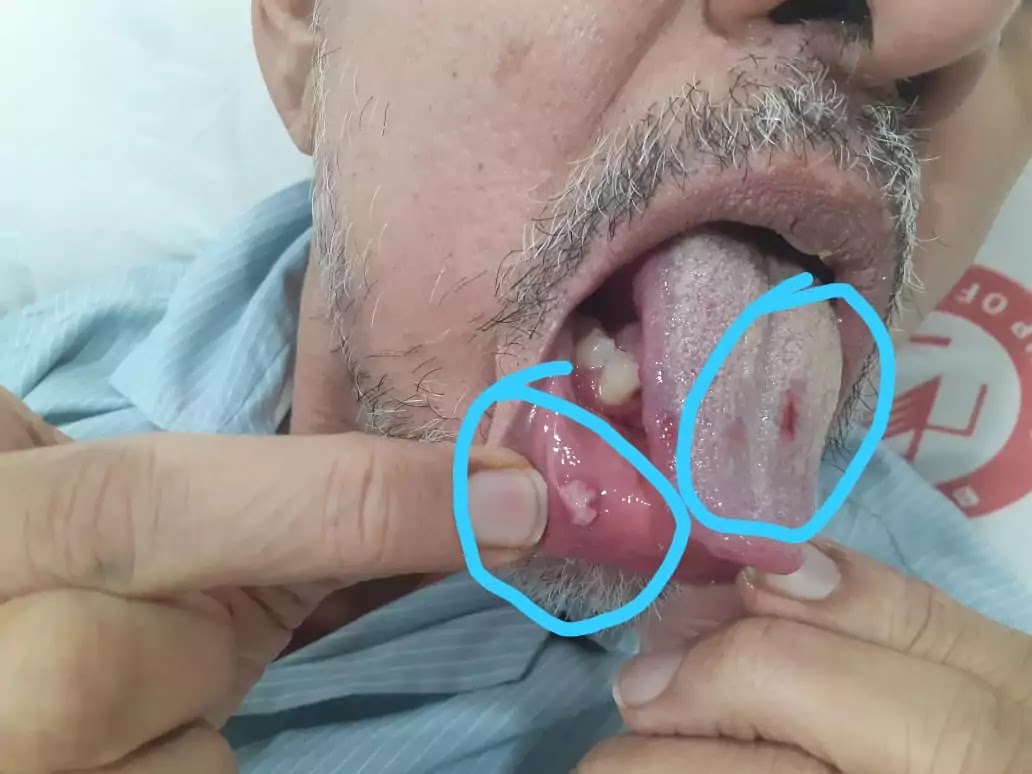
Kindly have a look at the image below and guess the diagnosis.
Diagnosis: Herpes ulcer and oesophagitis (Herpes simplex virus)
In this pandemic, there were many patients with dysphagia during or post COVID-19 illness or complications. The most common cause for that is Candida. Since there is a rise in the use of immunosuppressants, odd infectious diseases are coming up.
Back to our case:
He was started with intravenous acyclovir. Within 2 days there was significant improvement. The patient was discharged on oral valacyclovir for a further 3 days.
Learning points:
Painful ulcers on tongue or lips with dysphagia not responding to Fluconazole, then think about HSV that is Herpes Simplex Virus.
HSV summary
What is the herpes simplex virus?
As the name suggests it is a virus, also famous as herpes. It is divided into two types: Herpes simplex virus type 1 (HSV-1) and Herpes simplex virus type 2 (HSV-2).
HSV-1 is mostly represented as oral herpes and usually transmitted through contact with oral sores, saliva, and surfaces near the mouth. But it can also spread from the genital area via oral-genital contact.
HSV-2 is also called genital herpes and transmitted mainly via sex.
Both the infection remains lifelong and mostly asymptomatic. But when symptoms appear such as blisters or ulcers, it is excruciating. The risk of acquiring and transmitting HIV infection is also increased with HSV-2 infection.
For sharing such a wonderful educational case I once again thankful to:
Dr. Pratik Savaj
Infectious disease (ID) specialist
SCID-AI
(Surat Clinic of Infectious Disease and Adult Immunization)
Surat city, Gujarat, India